- Features
- No Comment
Aid cuts and a failed deal: Zimbabwe’s frontline health care under strain
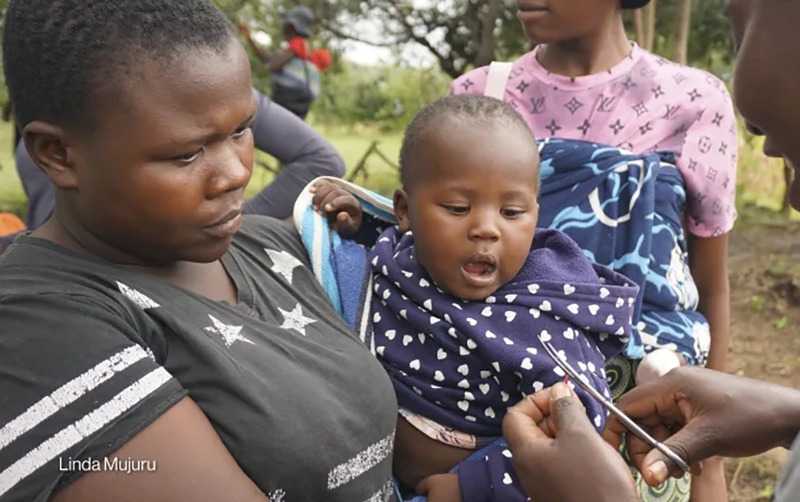
By devex.com
HARARE: In Gurure, a rural settlement about 140 miles (225 kilometers) east of the capital of Harare, 20 women sit on a rocky outcrop under the shade of a tree, their children gathered in their laps. They are waiting for the monthly health clinic to begin.
One community health worker, Melody Taasosa, 33, has already arrived in the village outside the town of Rusape. But she cannot begin weighing the children. The entire village relies on a single baby scale, and it is still on its way with her colleague, Portia Muswere, 29.
Both Taasosa and Muswere are community health workers, or CHWs, who are trained frontline providers delivering basic care at the household level.
As they wait, Taasosa turns the delay into a lesson. She teaches the women how to prepare nutritious porridge for young children, stressing the importance of adding protein.
“In maize meal porridge, you should add foods like eggs, fish, peanut butter, or even soya bean meal to improve the nutrients your child gets,” she says. “Cook it thoroughly and serve it while hot to avoid infections.”
Scenes such as this are common in rural Zimbabwe, where CHWs are often the first and sometimes only link between communities and the formal health system.
Much of the training, supplies, and program support sustaining Zimbabwe’s community health workforce has historically come from external donors, particularly the U.S. government. The largest funding stream was for the HIV and AIDS response under PEPFAR — the U.S. President’s Emergency Plan for AIDS Relief — which funds community-based testing, treatment adherence, and outreach.
PEPFAR has provided nearly $90 million each year toward salaries and incentives for about 21,700 health workers in Zimbabwe, including nurses, laboratory scientists, social workers, and CHWs, according to the U.S. Embassy in Zimbabwe.
Now, a convergence of shocks — sweeping U.S. aid cuts, the rollback of PEPFAR-supported programming, and the collapse of a proposed $367 million health agreement — has effectively cut off the main channels through which the U.S. funded Zimbabwe’s health sector. With no new agreement in place, the U.S. is winding down support, leaving organizations to scale back, frontline workers unpaid, and gaps in care widening across the country.
A failed health deal and threatened community care
In February 2026, Zimbabwe rejected a proposed memorandum of understanding with the Trump administration for a $367 million health funding package covering HIV and AIDS, tuberculosis, malaria, maternal and child health, and disease outbreak preparedness.
Zimbabwean officials called the agreement “asymmetrical,” citing concerns over sovereignty and data-sharing requirements.
As U.S. funding cuts take effect and no replacement agreement has materialized, more than 100 organizations that once sustained the community health workforce are scaling back or shutting down, according to a program officer with a local NGO funded through the U.S. government, who requested anonymity for fear of retribution.
Zimbabwe has an estimated 20,000 community health workers nationwide, according to a 2023 World Health Organization analysis, with around 15,000 supported by donor-funded NGOs.
The program officer said the effects are already rippling across the health workforce — from doctors and pharmacists to laboratory scientists, nurses, and counselors.
The program officer pointed to World AIDS Day commemoration in Zimbabwe as a stark example: In 2024, around 115 health organizations participated. A year later, just 11 were able to do so, as funding cuts sidelined the rest.
When a stop-work order halted PEPFAR programs in January 2025, community health workers and other staff supported through the initiative were forced to stop working. Many were never reinstated, as organizations scaled back or shut down due to funding losses.
While some PEPFAR support later resumed, it returned in a far narrower form. In Zimbabwe, funding continued only for essential services tied to antiretroviral, or ART, procurement, supported by a six-month, $65 million bridge fund from the U.S. government.
That funding expired in March 2026, and with a broader health financing agreement failing to materialize, there is little indication it will be renewed. Programs supported by this funding have also now ended, according to Donald Mujiri, a spokesperson for the Ministry of Health and Child Care.
The wider system that sustained HIV response, from community outreach and testing to staffing and support services, has not been restored, according to the program officer.
Zimbabwe’s Minister of Health Douglas Mombeshora announced soon after the 2025 funding halt that the government would absorb over 15,000 CHWs affected by the withdrawal of USAID support.
The process of adding community health workers to the government payroll is ongoing and not yet complete, according to Mujiri: “Remember, it’s not only community health workers who were impacted; even nurses, lab technicians, and others were affected, so the government is still working on absorbing all of these,” he said.
But more than a year later, that transition has yet to materialize, according to a program officer with a local NGO: “In that case, it means some target populations are no longer able to access services from community health workers. These workers serve different groups, some focus on children, others on high-risk populations such as sex workers,” she said.
The gap is significant. These frontline workers form the backbone of community-level health delivery, although authorities have indicated that the country still falls short of its target, with plans to scale up to as many as 40,000 health workers to ensure at least one health worker per village.

A strained front line
Community health workers in Zimbabwe are also on the front line of the fight against diseases such as malaria, diagnosing cases with rapid tests, treating uncomplicated infections, educating communities on prevention, and linking patients to local clinics for follow-up care. However, following stop-work orders from the U.S. government in January 2025, malaria cases surged.
According to the Ministry of Health and Child Care, from January to May 2025, cumulative malaria cases increased by 180%, and malaria-related deaths also rose by 218%. While multiple factors influence malaria transmission, government officials said the withdrawal of funding played a role in the surge.
Across the country, NGOs have long relied on community health workers and other community cadres to deliver U.S. government-funded health programming.
Community health workers such as Precious Musindo, a sex worker working with Springs of Life Zimbabwe, a community-based organization focused on supporting fellow sex workers, said the support they once offered has already diminished.
“CHWs used to receive allowances and airtime each month for their work. They provided counselling, reproductive health services, and empowerment initiatives, but all that is no longer feasible because of funding cuts,” she said.
Musindo said Springs of Life is still operating, but now entirely voluntarily, without funding. Their programming had previously been supported by the U.S. government.
Daniel Ngorima, a CHW in Rusape since 2015 who has worked for both the Zimbabwean government and U.S.-funded organizations, said he has also seen supplies diminish in the past year, including the small $45 stipend he used to receive each quarter.
“I provide blood pressure testing and health education at gatherings like funerals. We used to receive bags, uniforms, and other items from the U.S. government, but that has since stopped,” he said. “I will continue with this work despite not being paid because I am now accustomed to it, and people rely on me. I don’t want to let them down.”
Itai Rusike, executive director of the Community Working Group on Health, a local NGO aimed at promoting a healthy community, said funding cuts have already limited critical activities.
“They have restricted refresher training and halted critical community work such as malaria prevention, as well as maternal and perinatal audits,” he said of the funding shortfall.
A call for political will
Even as uncertainty grows at the national level, community health workers are already mobilizing to adapt. In Harare, over 90 CHWs gathered at a local clinic in March 2026 for a training session to strengthen their collective response to funding cuts.
The participants included a diverse group working under the Ministry of Health and Child Care, as well as those under various nongovernmental organizations that collaborate with the ministry on specific health priorities.
These cadres include peer educators, counsellors, male health advocates, and adolescent health workers. While each traditionally focused on a specific role, the meeting aimed to broaden their scope and better serve community needs.
Participants agreed to move away from strict specialization, with CHWs taking on a wider range of services — from maternal health advice and referrals for conditions such as high blood pressure to education on sanitation, nutrition, and immunization.
The shift allows them to address multiple needs in a single visit, improving access to care while making better use of limited resources. But it also means CHWs are taking on more work without additional pay. Many said they accepted the change out of a shared commitment to serving their communities.
Rusike noted that community health workers have historically been central to Zimbabwe’s primary health care system. However, he warns that their role has weakened over time, partly due to the absence of sustained domestic funding.
“There is no dedicated budget line for community health workers, which has led to overreliance on external partners. This is risky and unsustainable, as donors can withdraw support at any time,” he said.
At the policy level, uncertainty has deepened. The U.S., through a press release, announced it will begin winding down its health assistance to Zimbabwe after the government withdrew from negotiations on the health agreement.
In the statement, U.S. officials said their support has contributed more than $1.9 billion to Zimbabwe’s health sector since 2006, helping the country reach key HIV targets, including the UNAIDS 95-95-95 goals. Without a functioning health agreement, there is no clear channel for U.S. support to continue, according to several NGO officials.
Rusike said the solution lies in strengthening domestic systems: “If Zimbabwe is serious about revitalizing primary health care and achieving universal health coverage, community health workers must be prioritized,” he said. “Absorbing them into the government payroll system would strengthen service delivery and reduce dependence on external funding.”
The program officer who spoke with Devex on the condition of anonymity said the issue ultimately comes down to political will: “Without political will, it’s a big problem. But if there is commitment from the highest office, things can change,” she said.
Back in Rusape, health workers Taasosa and Muswere are already feeling the shift, with supplies dwindling. Recruited last year by the government of Zimbabwe, they have yet to earn anything.
Taasosa carefully lifts a baby onto the scale, resuming the clinic after the long wait. Despite challenges, she remains committed.
“I get to interact with other women when we do our work, share ideas, and learn. At the same time, I help my community, and that is fulfilling,” she said.